Herpes is an extremely common sexually transmitted disease (STD) that is rarely included in regular STD tests. Type 2, genital herpes, affects more than 13 per cent of Canadians, according to a 2011 study.
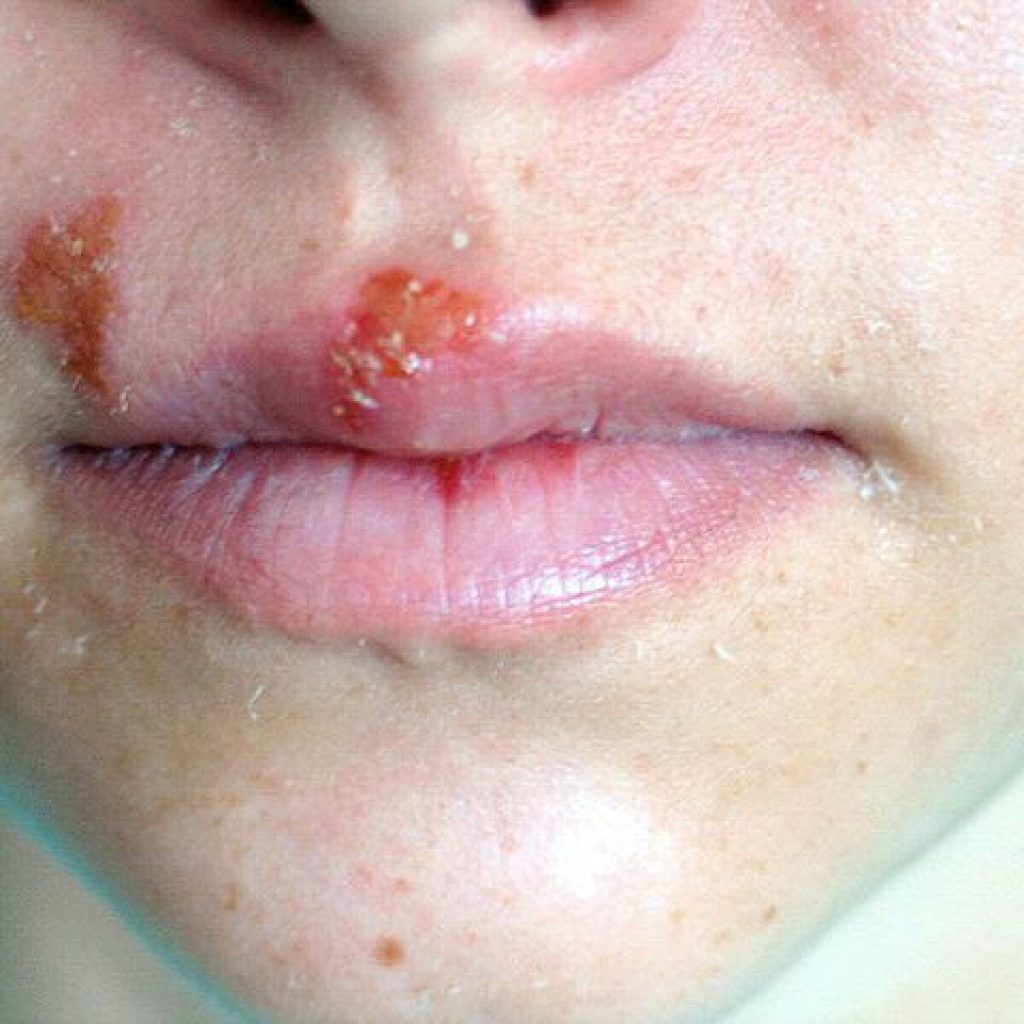
This study claims that type 1, oral herpes, affects approximately 66 per cent of the population. Ever had a cold sore? It’s herpes.
Simply getting tested for STDs following every new sexual partner, is not effective for conclusively diagnosing herpes.
Unless you describe herpes symptoms to your doctor, it’s unlikely that they would test for it.
Jennifer Burke is a sexual health counselor in Toronto. She said testing is limited in its scope because blood tests will come back positive if you’ve ever had contact with the herpes simplex virus (HSV) at any point in your lifetime.
If you’ve never experienced an outbreak you likely cannot transmit the virus to others and it will have no effect on your health. For these people, a diagnosis is not helpful in any way.

Diagnosing Genital Herpes
Genital herpes is typically diagnosed when patients are symptomatic. “They sit with a counselor or a nurse before seeing the doctor. And usually when they describe their symptoms, we prepare them,” Burke said.
She continued that the doctor will examine them and although they will still do tests, the doctor can diagnose them on speculation. “If the doctor sees something that looks like herpes, you’ll know right away,” she said.
The affected area is swabbed and doctors may do a blood test as well. Results take about a week, according to Burke.
Herpes does not affect overall physical well being aside from a general feeling of discomfort. Often, the psychological distress of an STD diagnosis is worse than the herpes virus itself.
Burke said patients are typically shocked when they learn they have HSV. She usually will have a conversation with patients about the social stigma around STDs and genital herpes and remind them to be kind to themselves.
Disclosing HSV to Sexual Partners
The stigma can make it difficult to work up the courage to tell a potential partner about your genital herpes diagnosis.
“I always say the best story to tell is the truth,” Burke said. “Bravely tell people and prepare yourself for rejection, unfortunately.”
She said that it likely will never get easier to tell partners. With practice, though, you’ll learn how you can best approach the situation.
Health Match provides some reassuring news that “treating the infected partner with suppressive therapy can prevent transmission of symptomatic herpes in over 90% of cases.”
Feeling anxious about your diagnosis? Read The Health Insider’s article about reducing anxiety through food.
Treatment
Burke said it’s important for people to know that although there is no cure for HSV, there are treatment options available.
She said antivirals can be taken at the onset of an outbreak. For those experiencing more than 5 or 6 outbreaks per year, there is suppressive therapy which can either decrease incidences or stop outbreaks altogether.
There are a few antiviral options. “Medications used to treat genital herpes include oral acyclovir, valacyclovir and famciclovir,” according to the Government of Canada.
Check with your insurance provider about your medications coverage.
“Start antiviral medications as soon as possible as they can reduce the duration of viral shedding, time to crusting and healing of lesions, duration of local pain and constitutional symptoms,” the government continues.
Since medications generally cannot be taken until you are experiencing symptoms, The Health Insider team compiled suggestions from Johns Hopkins Medicine and The Government of Saskatchewan for dealing with the associated pain and discomfort.
Johns Hopkins:
- Sit in warm water in a portable bath or bathtub for about 20 minutes. Avoid bubble baths.
- Keep your genital area clean and dry, and avoid tight clothes.
- Take over-the-counter medications, such as acetaminophen or ibuprofen. Avoid aspirin.
Government of Saskatchewan:
- Pat the area dry or use a blow‐drier on the cool setting on the area.
- If it hurts to urinate, pour water over your genitals while urinating or urinate in the bathtub.
- The use of creams or lotions on genital herpes is not recommended.
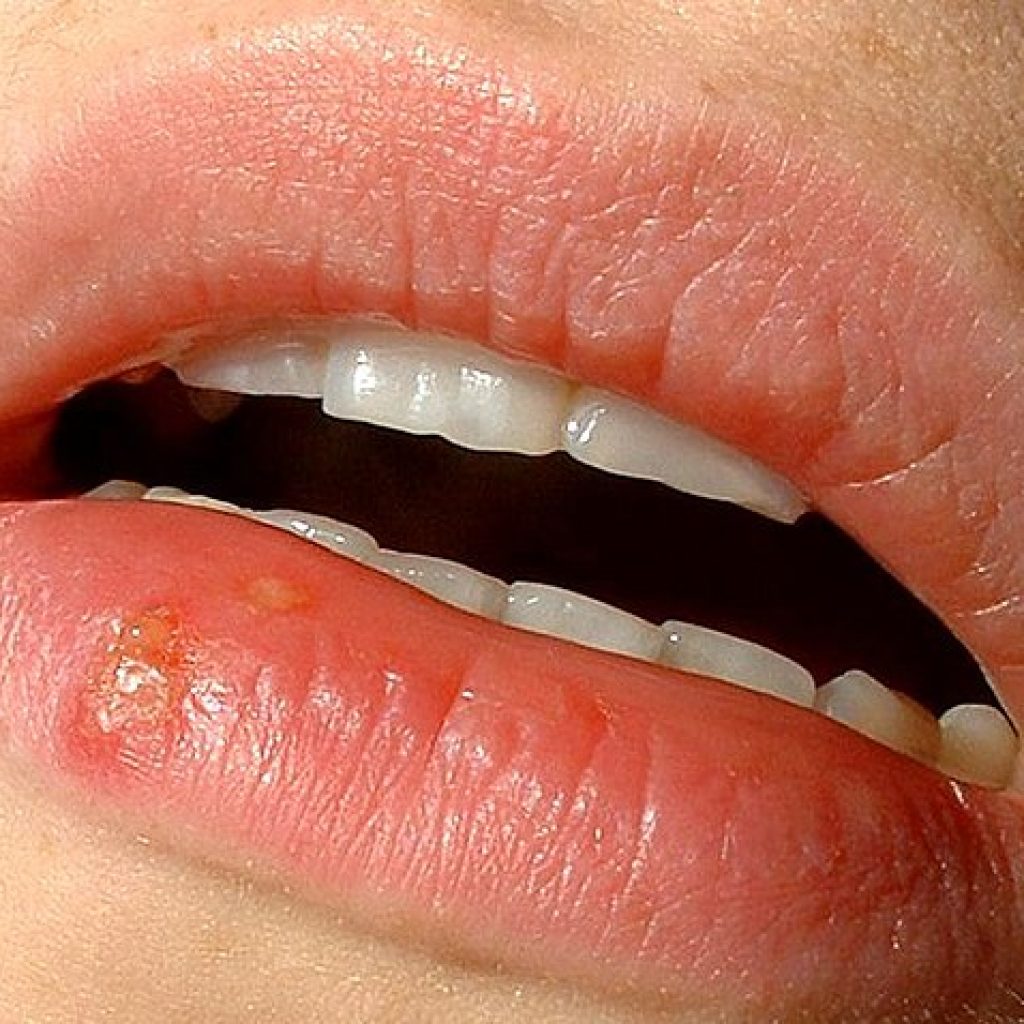
Bonus: Oral Herpes Treatment Option
For those willing to pay out-of-pocket, there is another option for treating oral herpes: the diode laser.
Laser therapy generally is not covered by insurance, according to Cleveland Clinic. Check with your insurance provider about coverage.
This process is typically done by dentists, so if you’re interested, call ahead and find out if your dentist can provide this service. If not, they may be able to refer you to a practice that can.
“The laser energy kills the surface virus, thus inactivating the lesion. In this process, nerve endings are cauterized, allowing the patient’s symptoms to resolve. The reduction in healing time is due to the process of photo biomodulation (PBM), a form of infrared light therapy at a specific wavelength that stimulates cells to produce natural healing and reduce pain,” according to Dimensions of Dental Hygiene.
New and/or Expecting Parents
Parents with HSV will need to be careful about not passing herpes on to their kids. Genetics are not a factor in contracting the virus, according to Health Match, but it can make you more susceptible to more frequent outbreaks.
Expecting parents should keep in touch with their doctor about the status of their condition. Notify your doctor of an outbreak near the baby’s due date.
Health Match says doctors will likely suggest a C-section if the birthing parent has a genital herpes outbreak during labour.
New parents can pass oral herpes on to children much the same way anyone can; namely through sharing food, drinks, utensils, kissing, and touching while experiencing symptoms.
Genital herpes can only be passed through genital contact while experiencing symptoms.
Herpes is extremely common in Canada and around the world. Knowing that HSV is typically a mild disease can help ease some of the mental burden of receiving a diagnosis.
If you’re struggling to wrap your mind around your diagnosis, try visiting a herpes support group in your area or join one online to connect with others experiencing the same problems.
The information provided on TheHealthInsider.ca is for educational purposes only and does not substitute for professional medical advice. TheHealthInsider.ca advises consulting a medical professional or healthcare provider when seeking medical advice, diagnoses, or treatment.










