Routine STI testing is essential to your health, but the embarrassing possibility of getting a positive result keeps many away from the clinic.
With chlamydia, gonorrhea, and syphilis rates on the rise, it’s increasingly important to stay on top of your sexual health screenings. Knowing if you have HPV is also important because of its link to cancer.
In reality, an STI is like any other infection, but these spread through contact with genitalia instead of a sneeze. Anyone who is sexually active should test for STIs every year or before sleeping with a new partner, whichever comes first.
If you have multiple partners or have partners with an unknown STI status, Health Canada recommends getting tested every three to six months.
While it’s always a good idea to let partners or potential partners know about a positive STI result, your tester will anonymously report chlamydia, gonorrhea, syphilis, hepatitis B and HIV to your local health department.
Don’t worry – you won’t get in trouble for having an STI. Rather, reporting is an important tool for public health. Also, a nurse will contact you to offer help telling your past and current partners that they need to get tested. This can also be done anonymously through reporting software if you’re too uncomfortable.
Navigate this Article
Chlamydia | Gonorrhea | Syphilis | Genital Herpes | Trichomonas | HPV | HIV | Hepatitis B and C
I Don’t Have a Doctor, Where Can I Get a Test?
Although a GP would be the quickest stop for an STI test, there are a couple of other options available to Canadians wondering about their status.
You can visit a nearby walk-in clinic or sexual health clinic. All STI testing, whether done through a GP or a clinic, is covered by Medicare. Some sexual health clinics offer free treatment for STIs as well.
Sexual health clinics also often have a bowl of free condoms by the front desk or door. Condoms are the best way to prevent a sexually transmitted infection; it never hurts to grab a few.
Canada’s Most Popular STIs and When to Get Tested
New partners might ask you to get an STI test before sleeping together the first time. It’s not because they think you’re dirty or overly sexually active, but rather it’s for their own sake of mind and sexual health regimen.
Below is a list of the most common STIs, their accompanying symptoms, along with indicators of whether they’re curable or simply treatable. Either way, testing is key.
Chlamydia – Curable
In the last decade, rates of infection have risen dramatically. Increasing by 33 per cent in Canada, it’s most likely to affect women aged 15 to 24. Not only can it be transmitted through vaginal, anal and oral sex, but it can also pass from mother to child during childbirth.

Routine testing is incredibly important because up to 60 per cent of people won’t show any symptoms and would otherwise have no idea they carry the bacteria.
If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Sexually active
- Under 25 years old
- Pregnant
Both men and women can provide urine to test for chlamydia along with a throat or rectal swab when applicable. Women may also be tested using a vaginal or cervical swab.
Health Canada recommends getting a test of cure three weeks after finishing treatment, especially if you didn’t manage to follow the directions to a tee.
Gonorrhea – Curable
Another STI with rapidly rising rates of infection, positive results in Canada have almost tripled in the last decade. Worryingly, it’s also becoming increasingly resistant to antibiotics, the usual treatment, which has resulted in the term ‘super gonorrhea’.
It is important to finish your full round of prescribed antibiotics, even after you feel better. Though you may be convinced that your body has cleared the bacteria, don’t count on it.
Some of the bacteria will have a slight resistance to the antibiotic already, especially if you’ve taken it before. Survival of the fittest, any bacteria that survives the treatment can then start to multiply, passing on their drug resistant properties.
Most likely to affect men aged 20 to 29, a disproportionate number of sexually active young adults test positive. Most women with gonorrhea will not show symptoms, though they can pass it on to their partners or their children during childbirth.
Gonorrhea can be spread through vaginal, oral, and anal sex.

If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Sexually active
- Under 25 years old
- Pregnant – first and third trimester
- Risk factors for blood-borne infections
Gonorrhea testing is done through a urine sample. You may be asked for a swab of the throat, cervix, anus, or penis.
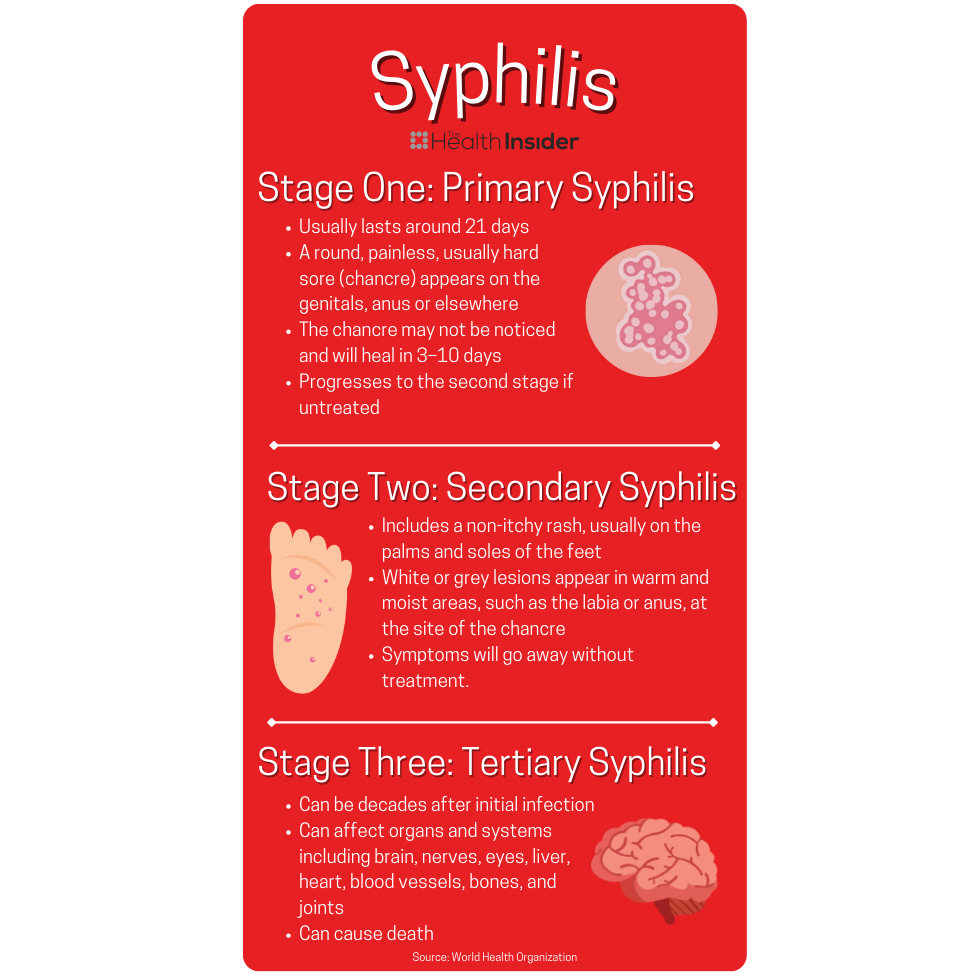
Syphilis – Curable
The last of Canada’s skyrocketing trio, syphilis infections in Canada have increased almost five-fold in the last decade.
The population most likely to contract the infection is gay, bisexual, and pansexual men. It can spread through vaginal, anal, or oral sex, sharing toys, from mother to child during pregnancy or childbirth, unscreened blood transfusions, or skin to skin contact with a sore/rash.
In Canada, all donated blood is screened and infected batches are discarded.
If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Sexually active
- Multiple partners and it’s been 3-6 months since your last test
- Pregnant
To test for syphilis, your health professional will take a blood sample.
Genital Herpes – Treatable
Globally, there has been a significant increase in genital herpes infections. It can be transmitted through vaginal, anal, or oral sex even if the person has no sores or symptoms. Though it’s possible, you are less likely to get an infection from an asymptomatic partner. It can also be passed from mother to child during childbirth.
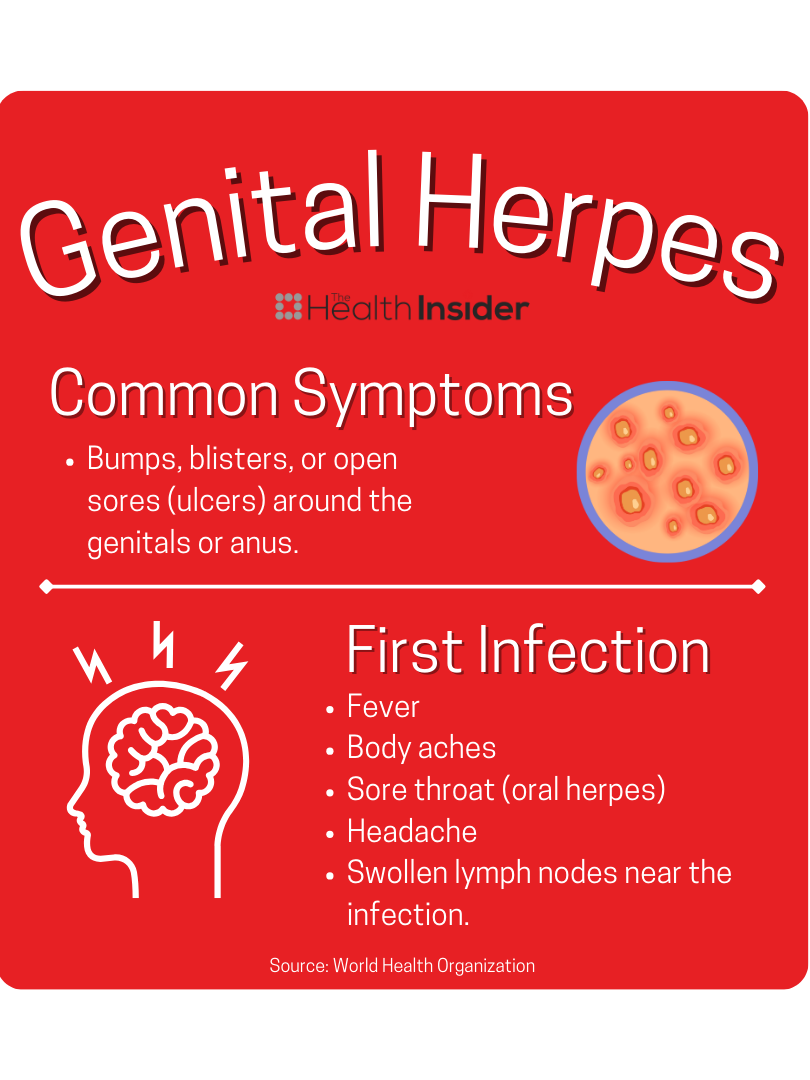
Herpes is an extremely common infection. In Canada, unless you specifically test for it and have experienced symptoms, your health professional likely won’t tell you about a positive result.
Read The Health Insider’s article to learn why: Not an Ingrown Hair: 13 per cent of Canadians Have Genital Herpes
If you have warts on or around your genitals, it’s time to get tested. Herpes can be tested using a blood sample or a swab of the sores. Though it can’t be cured, it can be effectively treated to reduce your chance of recurring symptoms. Some people on treatment never experience a second episode.
Health Canada recommends follow up appointments with your doctor if you experience a recurrence, if you’re pregnant, or if your doctor suspects drug resistance.
Trichomonas – Curable
Different from the other STIs listed, trichomonas (AKA trichomoniasis or trich pronounced ‘trick’) is not caused by bacteria. Instead, trich is caused by a parasite.
It’s the most common non-viral STI globally and is transmitted through vaginal, anal, and oral sex. Occasionally, it can pass from mother to baby during childbirth.
Up to 70 per cent of people won’t exhibit any symptoms, especially men. Trich disproportionately affects women.

Trich is passed on through vaginal, anal, or oral sex or through genital touching, even without ejaculation.
If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Assigned female at birth
- Sexually active
To test for trich, your health professional will take a swab of the affected area. They may also ask you for a urine sample.
HIV – Treatable
Hard to diagnose, HIV can present without any symptoms until AIDS develops, which can be up to 10 years after the initial infection. Luckily, new infection rates in Canada have been decreasing since 2017.
About half of people with HIV will develop mild flu-like symptoms two to four weeks after the infection.
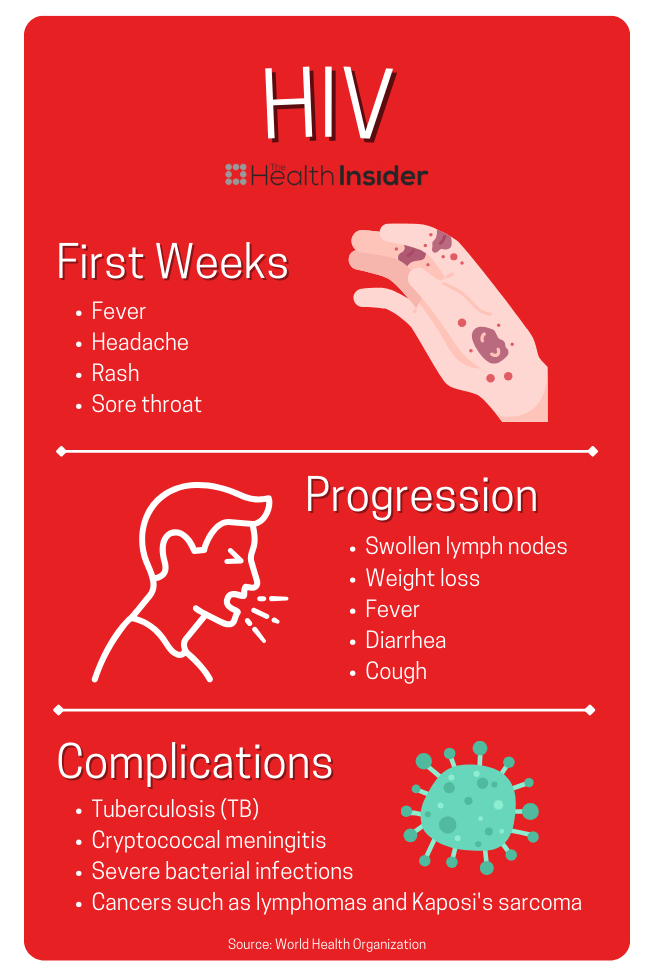
Currently, there is no cure for HIV, but it can be effectively managed with medications. 87 per cent of people who know their status are on treatment which suppresses their viral load. This suppression makes it extremely unlikely that a person can pass it on to their partner(s).
If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Men who have sex with men
- Sexually active
- Pregnant
Blood tests are used to diagnose HIV, though they may present a false negative during the first four weeks of infection, so it’s important to get tested multiple times.
HIV is highly contagious without proper medication and these first four weeks are no exception. If you suspect you could have HIV, take precautions to ensure you don’t pass it on.
HPV – Treatable
HPV is more common than many people may think. Health Canada writes that more than 70 per cent of Canadians (both men and women) will have at least one HPV infection during their lifetime.
It’s not technically curable since there are no medications you can take that kill off the STI; but that doesn’t mean you’ll live with it forever.
Especially if you’re 30 or younger, your body can clear the infection out all on its own in about a year. Unless there are painful symptoms like genital warts, you just have to wait for your immune system to do the work.
It’s very possible that without testing, you’ll never even know if you have HPV since it’s usually asymptomatic.
Passed through intimate skin to skin contact, it’s most often spread through vaginal, anal or oral sex. It’s very unlikely, but it is possible to pass HPV on to a fetus which can lead to complications in the child’s health.
If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Sexually active
- Have a vagina
There are 100s of different strains of HPV, but only a few of them are particularly dangerous. Children are immunized in school (or by a family doctor/walk-in) to prevent the spread of cancer causing strains.
Curious to know more about the link between HPV and cancer? Read The Health Insider’s article: HPV Screening Could Prevent Cervical Cancer
Testing for HPV can be done through a pap smear. Your health professional may use the same cervical cells collected to run the HPV test or they may take a second swab. Currently, there is no way to test men (or anyone without a vagina) for HPV.
Hepatitis B and C – Curable
Infection rates of hepatitis B and C have dropped significantly since 2019. Most likely to affect men aged 30 to 39, hepatitis also disproportionately affects underserved communities.
About two thirds of Canadians with hepatitis don’t know they have it, especially since symptoms may seem entirely random or not present at all.
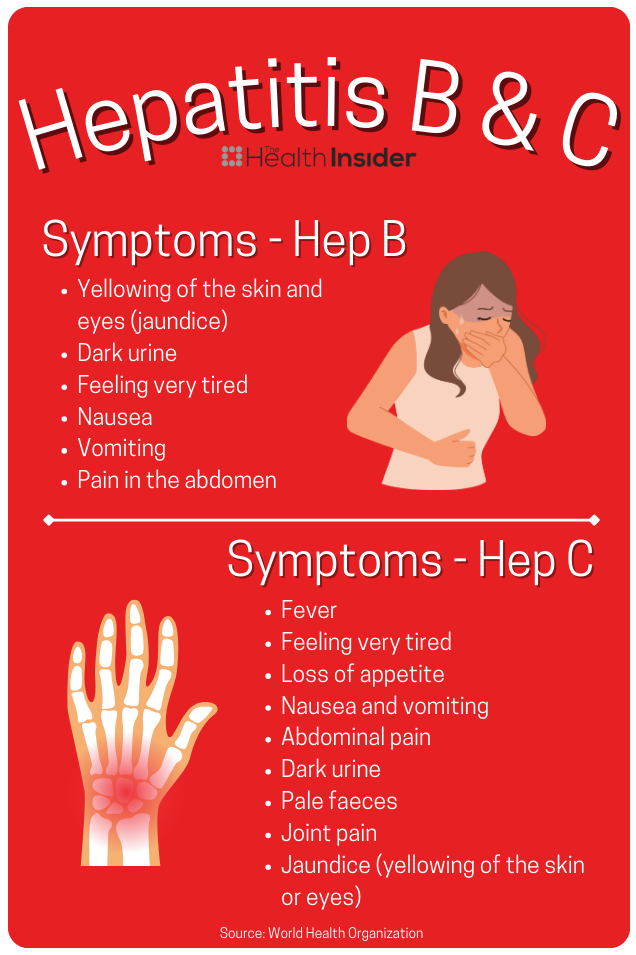
Hepatitis B and C can be passed on through vaginal, anal or oral sex, instruments that break the skin (like needles) or any exposure to infected blood or other bodily fluids. It can also be passed from mother to child during pregnancy.
If you fit the following criteria and/or are experiencing symptoms, it’s time to get tested:
- Indigenous
- Men who have sex with men
- Street involved youth
- Incarceration (past/present)
Testing for hepatitis is done through a blood test. Your body may be able to clear hepatitis B on its own, but it will not be able to clear hepatitis C.
Get Tested!
Having an STI can be embarrassing and scary. Your doctor can help you through the process of testing and treating the infection to ensure you make a full recovery when it’s possible and manage the symptoms when it isn’t.
Remember: if you’re sexually active, even if you don’t have any symptoms, you should get a full STI panel every year. If you have more than one sexual partner, you should get a full panel every three to six months or after every new partner.
With so many STIs possibly being asymptomatic, routine testing is crucial to maintain your sexual health and keep your partner(s) safe.
The good news is that every province has programs in place that make testing and addressing the issue as easy as possible, but you have to do your part. Get Tested.
~ Read more from The Health Insider ~
- Ditching your Sunscreen? Separate Fact From FictionTrading sunscreen for internet rumours exposes your skin to a proven Class 1 carcinogen — the sun. Read the risk analysis and learn about new options before heading outside.
- Would You Trust AI Over Your Doctor?Nearly half of Canadians use AI for medical advice, but 68% would still wait two weeks for a human doctor over an immediate AI diagnosis.
- Syphilis Is Surging in Ontario and Pregnant Women Are Paying the PriceOntario’s syphilis surge has reached every corner of the province. Here’s what pregnant people need to know about screening and protection.
- Red Light Therapy: Separating Science From HypeBeyond the wellness trend lies real clinical proof. Discover how red light therapy physically heals cells, targets chronic pain, and regrows hair.
- Beyond Ibuprofen: New Tech and Natural Remedies for Period PainPeriod pain isn’t just something you have to endure. Discover the natural remedies and Health Canada-approved tech that offer proven relief.
- PCOS Has a New Name and This is Why it MattersPCOS is now PMOS (Polyendocrine Metabolic Ovarian Syndrome). Discover why this landmark renaming matters for patient diagnosis and metabolic care.
The information provided on TheHealthInsider.ca is for educational purposes only and does not substitute for professional medical advice. TheHealthInsider.ca advises consulting a medical professional or healthcare provider when seeking medical advice, diagnoses, or treatment. To read about our editorial review process click here.