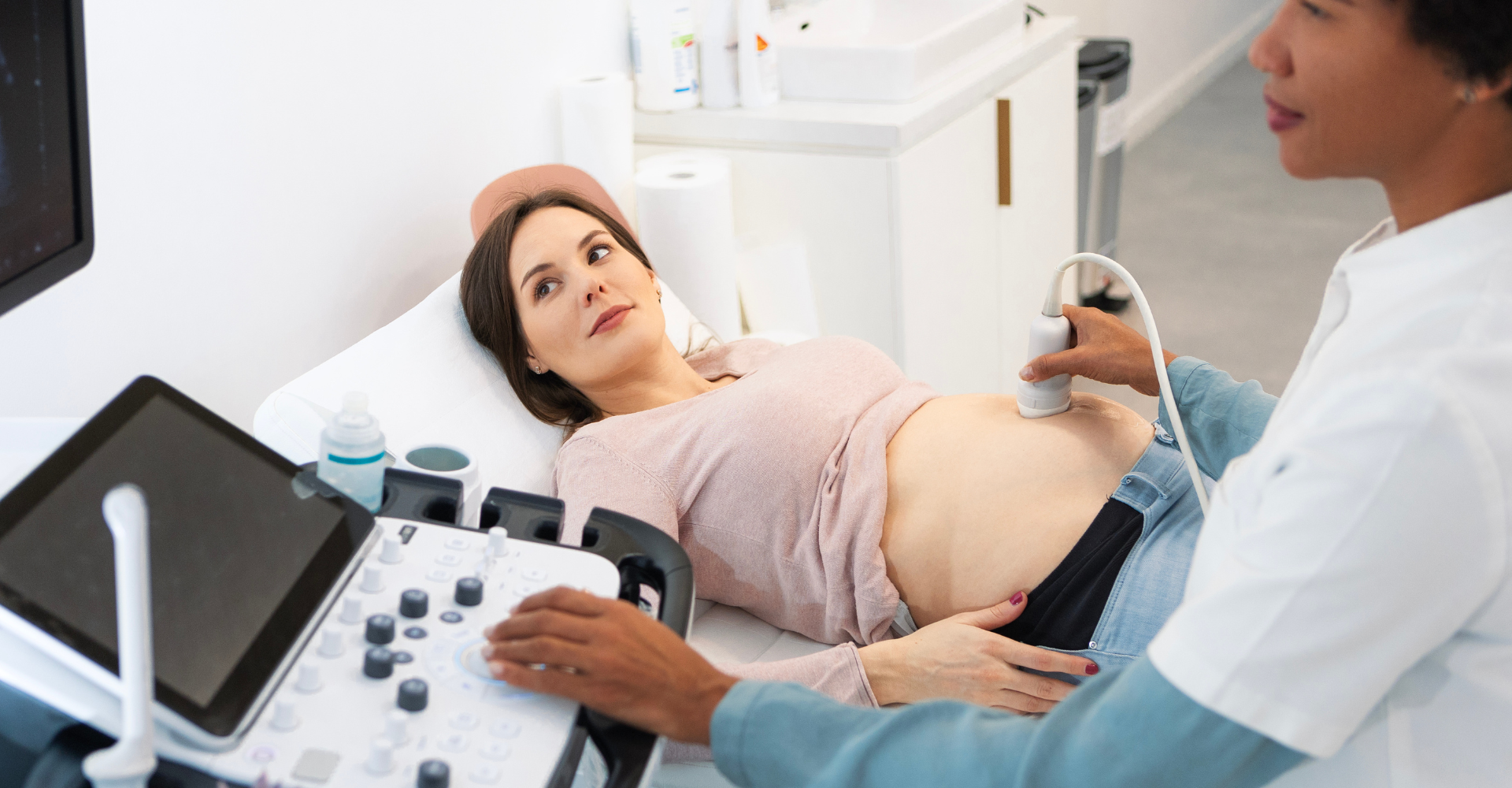
Deciding whether to have prenatal genetic testing is a personal decision with no right or wrong answer.
Prenatal genetic tests can identify whether your baby is more or less likely to have certain birth defects, or genetic disorders. The results of genetic screening can provide important information, but also can lead to difficult choices.
Some families wish to be armed with knowledge before birth that their baby will be born with a genetic disorder. This can give parents time to adjust to their new reality, and to learn about the disorder and caring for their newborn’s needs.

Other parents may decide not to have follow-up diagnostic testing if a screening test result is positive. Or they may decide not to have any testing at all or may simply not have access to screening.
Some parents may decide to terminate the pregnancy if they discover their baby has a life-threatening genetic illness.
Regardless, some prenatal genetic screening is available to women in Canada as a routine part of prenatal care.
Prenatal Genetic Screening
There are two types of prenatal tests for genetic disorders: prenatal genetic screening and prenatal genetic diagnostic tests. Prenatal genetic screening precedes diagnostic tests.
Testing for prenatal genetic illnesses is a journey with a number of stops along the way, ultimately informing you of the chances that your fetus has an aneuploidy and a few other genetic disorders.
There are two paths to finding out prenatally if your baby has a genetic illness. One is called Enhanced First Trimester Screening and the other is Non Invasive Prenatal Testing (NIPT).
Enhanced First Trimester Screening (eFTS)
Enhanced first trimester screening and is done between 11 weeks 2 days and 13 weeks 3 days of gestation. This test is different from the typical “dating” ultrasound done in the first trimester to ascertain due date.
It is performed through a Fetal Nuchal Translucency Ultrasound as well as a blood test. These tests can provide an indication as to whether your baby has Trisomy 21 or Trisomy 18. If you are given a positive result, you can then choose to carry on with prenatal diagnostic testing.
Second trimester genetic screening (STS) tests for the same genetic illnesses as eFTS but only through a blood draw done between 14 weeks and 20 weeks, 6 days.
Non-Invasive Prenatal Testing (NIPT)
Non-Invasive Prenatal Testing (NIPT) differs from Enhanced First Trimester Screening in a number of ways.
It can be done earlier, from the 9th or 10th week of gestation onwards, depending on the lab. It is done only through blood work and it tests for Trisomy 21, Trisomy 18, Trisomy 13 and +/- sex chromosome differences.
An 18–22-week ultrasound is recommended for extra information about the baby’s health.
NIPT is the most accurate genetic prenatal screening test. However, while they are highly accurate tests, neither eFTS nor NIPT’s can tell whether a fetus actually has a genetic illness. Only a diagnostic test can do this.
Prenatal Diagnostic Tests
Prenatal Diagnostic tests can tell you definitively whether your fetus actually has certain genetic disorders. They are done on cells from the fetus or placenta obtained through amniocentesis or chorionic villus sampling (CVS).
Amniocentesis is usually done between the 15th and 20th week of pregnancy while chorionic villus sampling is done during early pregnancy, most often between the 10th and 13th weeks.
Diagnostic tests carry a .5 to 1 per cent risk of miscarriage.
The results from first-and second-trimester tests can be useful when combined as they are more accurate than a single test result. If you choose to proceed with combined screening, keep in mind that final results often are not available until the second trimester.
Carrier Screening
If you suspect that you or your partner are carriers of a genetic disorder, carrier screening may be the right choice for you prior to conceiving, or during pregnancy if desired.
It is done via a simple blood or saliva test to determine if you and/or your partner carry genes that could increase your chances of having a baby with a specific genetic condition.
Inherited disorders include cystic fibrosis, Tay-Sachs disease, fragile X syndrome, some anemias, hemophilia, thalassemia and others. In most cases, both parents must carry the same gene to have an affected child.
Carrier testing is not to be taken lightly. To help prepare you, your doctor may have you talk to a genetic counsellor to help you understand the test and learn what the results could mean.
Furthermore, testing is not 100% accurate, however if you are in one of the higher-risk ethnic groups, testing is more accurate for certain diseases.
Cost
Most provinces publicly fund eFTS, check with your healthcare provider or provincial government to be sure. If you don’t have a healthcare provider, visit a local walk-in clinic to get a referral to the nearest maternity program in your area
As of today, only Ontario and Quebec offer publicly funded NIPT, and only for high-risk pregnancies. High-risk pregnancies are defined as: maternal age over 40 years, a family history of trisomies 21, 18, and 13, or a twin pregnancy.
In all other provinces, NIPT tests are available as an out-of-pocket expense. If you have private insurance, check with your insurance provider to see if they will cover NIPT.
Depending on the province and funding criteria, carrier testing may be covered. Check with your provincial health department to see if you qualify.
Carrier testing is available privately in Canada through Genolife or Lifelabs for those who can pay out of pocket.
95 to 99 per cent of women who go through with NIPT receive negative results, so if you do decide to go through with genetic testing, rest assured that most of the time, the news is good.
The information provided on TheHealthInsider.ca is for educational purposes only and does not substitute for professional medical advice. TheHealthInsider.ca advises consulting a medical professional or healthcare provider when seeking medical advice, diagnoses, or treatment.