My mother has suffered from dry eye for many years, and was recently diagnosed with Dry Eye Disease (DED). With about 21% of Canadians suffering from DED, she’s not alone.
While not usually serious, DED can profoundly impact a person’s life.
In the case of my mother, she no longer reads books as they irritate her eyes. Instead, she listens to audio books. Streaming and watching her beloved tennis tournaments on her computer or playing Bridge is also hard on the eyes, but she has no intention of stopping these activities.
In fact, she found a treatment just in time for the Grand Slam season that worked for her. I’ll go through the details a bit later in this article.
In the meantime, let’s examine what causes dry eye, its symptoms, and treatments available here in Canada.
What is Dry Eye Disease?
Dry eye occurs when your eyes do not make enough tears to stay wet, or when your tears don’t work correctly.
Tears are created in lacrimal glands (also known as tear glands) located in the upper outside corners of your eyes. They’re comprised of mostly salt and water. This fluid moves across your eyes as you blink and is mixed with oil from your meibomian glands to form your tears.
If left untreated, chronic dry eyes can damage, and possibly scar the corneal tissues of the eye, potentially leading to vision impairment. Additionally, as dry eyes can increase eye irritation, wearing contact lenses can be difficult for people with DED, and can increase the potential for developing an infection.
Symptoms and Causes
The symptoms of dry eye are as one would expect. Red, burning eyes that feel like sandpaper are often reported, with light sensitivity or blurred vision. Some people suffer from excessive tearing, which is an unintuitive, but real symptom.
According to the Canadian Association of Optometrists, a lot of things can cause dry eye, some of which you can control and some of which you cannot. For example, genetics and family history are now thought to play a role in dry eye so make sure you inform your doctor about any known cases in your family.
Many kinds of medication can cause DED. These include:
- Accutane
- Diuretics
- Decongestants
- Some blood pressure lowering drugs
- Oral contraceptives
- Antihistamines
- Antidepressants
- Anti-nausea medications
- Anticholinergics
Your doctor or pharmacist can educate you on which specific medications may worsen dry eye.
Illness can also cause DED, including Sjogren’s syndrome, allergic eye disease, rheumatoid arthritis, lupus, scleroderma, graft vs. host disease, sarcoidosis, diabetes thyroid disorders or vitamin A deficiency.
Hormonal fluctuations during menopause, pregnancy and menstruation can also contribute as can excessive screen time, pollution, smoke, dry air, previous eye surgery, and lifestyle choices such as smoking.
Aging and some eye makeup products are also culprits.
Dry Eye Treatments
Dry Eye Disease is a chronic complex condition that is challenging to treat. Since the origin of the disease can be from multiple sources, it may be necessary to try different therapies before landing on the one that works for you. Below you’ll find some common treatments to explore with your medical team:
Vitamins B12, D, and Omega 3’s have been shown to help with DED. Some doctors prescribe fish oil however recent research has found no benefit of fish oil supplements for dry eye prevention or treatment.
Eye drops – be careful with random eye drops purchased at the drug store. The wrong eye drops can wash away the vital protein, lipids and mucus that create a healthy tear film and prevent tear evaporation.
This, along with chemicals present in some popular eye drops, can make dry eye symptoms much worse over time. It’s important to work with your doctor to get the best eye drop prescribed specifically for your needs.
Following is what is typically prescribed in Canada:
- Corticosteroid eye drops: Used if there is an inflammatory component for a short time only.
- Cyclosporin eye drops: Used for long-term treatment. May take 3 months or more before relief is experienced.
- Lifitegrast eye drops for moderate inflammation.
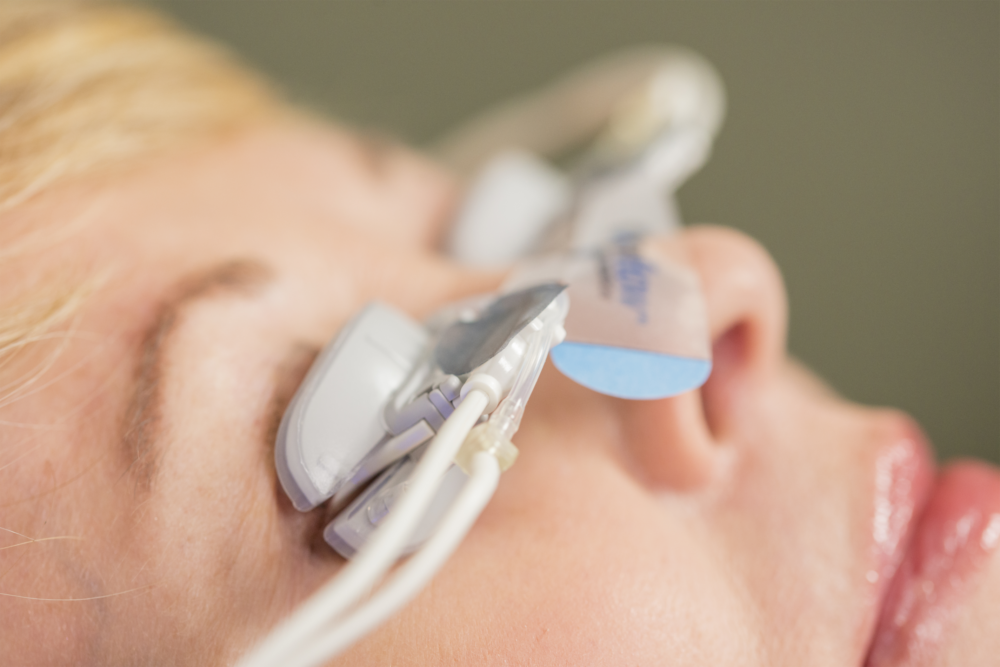
Intense pulsed light (IPL) therapy can successfully treat DED symptoms caused by inflammatory dry eye. Long term studies, however, indicate that the result is temporary with effects gone after nine months.
LipiFlow treatment combats problems affecting the meibomian gland, delivering heat and pressure to the meibomian glands to eliminate blockages and promote increased production and flow of tears.
Punctal plugs, about the same size as a grain of rice, are placed in the punctum, the entry to the tear duct.
Lifestyle
Lifestyle choices can play a significant role in causing DED. While many things such as pollution including the smoke from wildfires are out of your control, there’s a lot you can do to help dry eye from worsening.
Smoke, wind, and air conditioning can wreak havoc with dry eye. Try to avoid air conditioning blowing directly on you. Wear protective eyewear if outside on a windy day. During wildfire events or if you’re in an environment with significant air pollution, stay indoors as much as possible. Use air filters indoors and ensure that as little of the external air as possible is entering the building.
Use a humidifier in your home to keep the air from getting too dry. This is particularly important for Canadians and our cold, dry, long winters. Drink plenty of water, especially during the dry winter season.
Avoid cigarettes and cannabis as they can both cause dry eye.
Computer Eye
One of the most egregious “lifestyle” culprits in the dry eye story is computer use.
Computers and display devices with screens such as iPads and mobile phones decrease the number of eye blinks, leading to incomplete blinking, evaporation of tears, and potentially to dry eye disease.
But there are things you can do to help avoid dry eye due to computer use. Try these tips:
1.Raise your chair or lower your screen 15 – 20 degrees down from your eyes. This will lower your eye lids and decrease the dryness associated with more open lids.
2.Adjust the brightness of your computer screen, generally to about the same brightness level as your environment.
3.Increase the font size of your screen so you need to focus less.
4.Change the font itself. Fancy fonts are wonderful, but sans serif fonts tend to be more comfortable to read.
5.Try the 20-20-20 rule. Every 20 minutes look at something 20 feet away for 20 seconds.
At-Home Remedies
Unfortunately, diagnosis and treatment of DED is not covered under any provincial medicare, but it may be covered under most private insurance plans. There are however quite a few things you can do inexpensively at home to help with dry eye.
In the case of my mother, after receiving treatment for glaucoma, which was covered by medicare at a private clinic, she was offered a free Dry Eye Disease examination.
The clinic confirmed that she suffered from DED and recommended that she proceed with Lipiflow treatments to help with her blocked meibomian glands.
She was informed that the treatments would cost $300 per session and that she would need 4 sessions over the course of a year, with a treatment every six months after that for maintenance.
As an elderly retiree with only government health insurance, she could not afford to get the recommended treatment. Instead, she followed the advice proffered by the nurse at the clinic who advised my mother to try using heat treatment on her own at home if she could not afford the clinical sessions.
Ever intrepid, my mother soon realized that a warm towel or compress didn’t keep the heat long enough to make a difference. After researching what is available for at-home heat treatment online she purchased a heated eye mask device which she uses on her eyes for 15 minutes at 45 degrees before going to sleep.
She also uses the mask in the day as needed if her eyes are uncomfortable. The at-home treatment, along with humidifiers, medicated eye drops to keep allergies at bay, and taking a daily fish oil capsule has made a dramatic difference in keeping her eyes hydrated.
While there is no cure for dry eye, there are many options available to help alleviate your suffering that won’t break the bank. Don’t allow dry eye to rule your life!
The information provided on TheHealthInsider.ca is for educational purposes only and does not substitute for professional medical advice. TheHealthInsider.ca advises consulting a medical professional or healthcare provider when seeking medical advice, diagnoses, or treatment.